Optics, Electronics Combine for Non-Invasive, Accurate Arthritis Assessment
You’ve undoubtedly seen the finger clip-on device that measures peripheral capillary oxygen saturation (SpO2) in real time, using a pair of LEDs, a phototransistor, sophisticated electronics, and complex algorithms. You can now buy one for about $20 at almost any drug store.
This non-invasive electro-optical unit has completely obsoleted the frustrating, time-consuming, labor-intensive, invasive, and costly previous technique that involved physically taking a blood sample and sending it out for test. It was one of the first devices in the trend to use the synergy of developments in optics, electronics, and computing to provide medical tests that are convenient, minimally disruptive, often non-invasive, yet accurate.
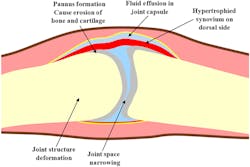
A recent effort expands on this use of multiple wavelengths of light to determine if a patient has rheumatoid arthritis (RA), an autoimmune disease in which the body’s immune system attacks the lining of joints, causing painful inflammation and swelling (Fig. 1).
1. This is the joint of a rheumatoid arthritis (RA) patient with inflammation on the dorsal (back) side. (Source: University of Birmingham – UK)
The work, being done by a team at University of Birmingham (UK) School of Computer Science with various medical institutions as partners, combines 3D digital imaging with infrared spectroscopy. The goal is to create a 3D image of blood content inside a patient’s hand and joints that can be used to produce an objective, quantifiable assessment. In theory, this could replace the current diagnosis approach that relies on a complicated combination of physical examinations by a rheumatologist, blood tests, and scanning by x-ray or ultrasound—all of which is time-consuming, subjective, and requires highly trained staff.
Since oxygenated and deoxygenated blood absorb light differently, it’s possible to use the infrared imaging to calculate warning signs of RA, such as lowered levels of blood oxygen (hypoxia) and increased levels of blood content in the joint—indications of inflammation. The team used both British and U.S. standards, which differ somewhat, in assessing RA severity.
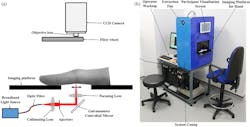
In their noncontact diffuse-optical-imaging (DOI) system, patients place their hand on the platform of the unit, and a broadband point source of light at five wavelengths (650, 710, 730, 830, and 930 nm) was directed into the joint (Fig. 2). On the opposite side of the joint, optical transmission images of the finger were collected at 14 positions using an air-cooled, charged-coupled device (CCD) camera, with spectral decoupling accomplished via a filter wheel preceding the camera objective lens.
2. Shown is a schematic of system for acquisition of dorsal optical-transmission images (a). In the optical-imaging system setup, patients place their hand on the imaging platform and align their finger joint of interest with the source prior to the acquisition of optically created data (b). (Source: University of Birmingham – UK)
The acquired data requires significant processing to be useful, including data-derived adjustable thresholds, masking, filtering, and fast Fourier transforms (FFTs). All data reduction and statistical analysis is done using MathWorks’ MATLAB.
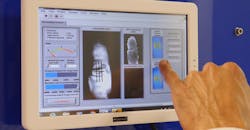
Dorsal (rear) optical transmission images of two fingers of one test subject illustrate the typical optical contrast observed between inflamed and noninflamed joints (Fig. 3). The left image shows an area of lower intensity at the joint region compared to the immediately surrounding finger surface (and which was clinically inflamed according to U.S. measurements), while the right image shows a peak of intensity at the joint region of a healthy finger.
3. Results of imaging of two finger joints come from the same participant. The top row shows the optical dorsal transmission images at 650 nm when the point source is directly under the joint, overlaid on a brightfield image of the finger. The second row shows corresponding line profiles of the mean intensity in the transverse direction. (Source: University of Birmingham – UK)
The test apparatus and associated pilot study data and conclusions are displayed as boxplots (Fig. 4). This pilot study involved 144 joints from 21 rheumatology patients. There was significantly higher median FFT amplitude for inflamed joints compared to noninflamed joints (with both U.S. and British criteria). The system demonstrated accurate detection of inflamed joints, with results that closely matched diagnoses made using conventional ultrasound and clinical examination approaches.
4. Example boxplots for the FFT amplitudes compare noninflamed versus inflamed joints, labeled using both British (CE) and US RA criteria (a), and joints from the RA patient group with those from the non-RA group (b). (Source: University of Birmingham – UK)
The full research paper “Detecting inflammation in rheumatoid arthritis using Fourier transform analysis of dorsal optical transmission images from a pilot study” was published in the Journal of Biomedical Optics, a publication of SPIE (the international society for optics and photonics). Also, check out this brief video:
About the Author

Bill Schweber
Contributing Editor
Bill Schweber is an electronics engineer who has written three textbooks on electronic communications systems, as well as hundreds of technical articles, opinion columns, and product features. In past roles, he worked as a technical website manager for multiple topic-specific sites for EE Times, as well as both the Executive Editor and Analog Editor at EDN.
At Analog Devices Inc., Bill was in marketing communications (public relations). As a result, he has been on both sides of the technical PR function, presenting company products, stories, and messages to the media and also as the recipient of these.
Prior to the MarCom role at Analog, Bill was associate editor of their respected technical journal and worked in their product marketing and applications engineering groups. Before those roles, he was at Instron Corp., doing hands-on analog- and power-circuit design and systems integration for materials-testing machine controls.
Bill has an MSEE (Univ. of Mass) and BSEE (Columbia Univ.), is a Registered Professional Engineer, and holds an Advanced Class amateur radio license. He has also planned, written, and presented online courses on a variety of engineering topics, including MOSFET basics, ADC selection, and driving LEDs.
Voice Your Opinion!
To join the conversation, and become an exclusive member of Electronic Design, create an account today!

Leaders relevant to this article: