Lightning Bolts, Defibrillators, And Protection Circuitry Save Lives
Victims of sudden cardiac arrest (SCA) can be saved with a small, prompt lightning bolt (i.e., a defibrillator shock) to the chest. The shock (3 to 5 kV and 50 A) stops the heart from unproductive fluttering (fibrillating), which fails to pump blood to the brain and other organs. It also allows the heart to restart orderly pumping of blood.
Hospitals often monitor the heart using an electrocardiograph (ECG) with a separate defibrillator. The ECG leads (i.e., electrodes) are on the patient when the defibrillator delivers the shock. With no warning, the ECG must withstand this lightning bolt and continue working properly.
This file type includes high resolution graphics and schematics when applicable.
According to the American Heart Association (AHA), nearly 383,000 out-of-hospital sudden cardiac arrests occur annually, and 88% of cardiac arrests occur at home. Sadly, less than 8% of people who suffer cardiac arrest outside the hospital survive.1 In medical terms, a heart attack and an SCA are very different. An SCA has no warning signs. People just collapse. Multiple, generally understood warning signs precede a heart attack.
Without our protective skin, the heart is vulnerable to very small currents. In the electrically susceptible patient, moreover, even minute amounts of current (10 μA) can cause ventricular fibrillation.2 Remember that with an ECG and a separate defibrillator, several pieces of equipment can be attached to the patient at the same time. Clearly, the total leakage current must remain below the threshold that can harm a human heart.
Defibrillators And Life-Saving Shocks
Many think that a defibrillator restarts the heart, but actually it stops the heart. There is a random beating in the heart called fibrillation, which means the heart is not coordinated and not pumping blood. The defibrillator shocks the heart into inactivity, allowing the normal sinus rhythm to restart.
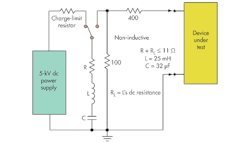
A hospital-grade defibrillator produces 3- to 5-kV voltage and 50-A current to penetrate the chest and shock the heart (Fig. 1). High voltage and current are necessary because the human body is ~75% salty water. The body conducts most of the electricity away, bypassing the heart.
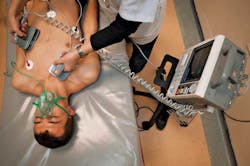
Automated external defibrillators (AEDs) are designed to be used by members of the public with minimum training (Fig. 2). These disposable electrode patches serve two purposes: first, monitor the heart with an ECG; and second, apply the high-voltage shock.
The AED protects its own input from the high voltage and current shock because it knows when it is about to apply the shock. Therefore it can, and does, disconnect the ECG monitor during the shock. The hospital-style defibrillator, however, is often used with a separate ECG or monitor. The ECG or monitor has no advanced warning and must withstand the high voltage and current of the shock.
Protecting The Defibrillator For ECGs
The voltage produced by a hospital defibrillator might be 3 to 5 kV at 50 A. A defibrillator test set looks very much like the standard ESD test set (Fig. 3).3 There is, however, an important difference. The ESD test has a capacitor measured in picofarads, but the defibrillator test set is in many microfarads. So, the extra energy from the defibrillator must be dissipated in front of the ECG.
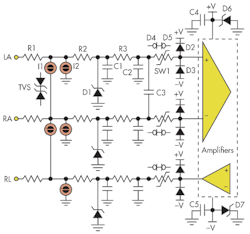
Figure 4 shows a defibrillator’s typical protection circuitry for an ECG. For convenience, we labeled the components in the left arm (LA) input circuit at the top. The normal ECG waveforms are on the order of a few (0.5 to 7 mV) millivolts, but the high-voltage defibrillator is in kilovolts and can last 5 to 20 ms, which is a long time for electronic components to survive such high voltage.
Most ECG front ends use neon glow lamps such as the NE-2 or NE-23 (I1 and I2) for protection. A small radioactive dot inside the NE-23 provides photons to stabilize the ionization voltage. Alternatives for the neon lamps include gas-discharge arrestor tubes and transient voltage suppressors (TVSs).
Resistor R1, in the range of 10 to 20 kΩ, can be in the input of the amplifier or built into the cables. It is the series element that limits the current in the neon lamps. Resistors R2 and R3, along with capacitors C1, C2, and C3, form lowpass filters. The D1 diode limits the voltage to a lower level. D1 can be a zener or avalanche diode, a metal-oxide varistor (MOV), or a thyristor surge protector. The D1 capacitance in conjunction with C1 is part of the lowpass filter.
Capacitor C2 is the common-mode filter, whereas C3 provides differential filtering. Typically C3 is about 10 times larger than C2. SW1 is a high-voltage signal-line protector: a switch that senses high-voltage, turns off the series switch, and turns on a clamp to reduce the amount of voltage at the amplifier. SW1 can be replaced by a current-limiting diode that looks like a JFET with the source and drain terminals tied together.
Diodes D2 and D3 are ESD-protection (electrostatic discharge) diodes that clamp the amplifier input to the power supplies. Notice C4 and zener diode D6 at the top of the amplifiers. They absorb and clamp the positive voltage rail. C5 and D7 do the same for the negative power rail.
Nothing is perfect, though. This ECG defibrillator protection circuitry involves tradeoffs between how well the amplifiers are protected and the frequency response necessary for the ECG to function properly. The capacitance of the protection devices is critical to preserve the wanted heart frequency response.
Repeated defibrillator shocks can degrade the input devices. The electrode degradation can contaminate the neon lamps, and the defibrillator’s glass envelope can break to allow air and water into the lamp. Consequently, most manufacturers recommend replacing the input protection devices at least annually. In a hospital setting where the ECG and defibrillator are used frequently, they receive more shocks and will degrade even faster.
Now we must consider the effects of ESD as well as radio frequency interference (RFI), electromagnetic interference (EMI), and susceptibility (EMS) on this protection design.4 The devices in Figure 5 fall into three categories:
• Voltage-limiting devices: gas discharge arrestors, MOVs, suppressor diodes, triacs, diacs, and switches
• Current-limiting devices: fuses, circuit breakers, and thermal cutouts
• Risetime reducers: resistors, inductors, coils, ferrite beads, and capacitors, all of which slow the risetime of a transient and, thereby, allow time for other protection devices to function
Capacitors are used with the resistors, ferrite beads, and inductors to act as lowpass filters. This approach controls the anti-alias filtering for the data converter. It slows the ESD risetime by spreading the impulse over time and allows the capacitors to be more effective.
The working voltage, equivalent series resistance (ESR), and self-resonance point of each capacitor need to match the application’s frequency and bandwidth. The self-resonance point may mean that several smaller resistors are necessary in parallel to absorb the fast risetime of ESD and a defibrillator shock pulse.
Each of these networks is reciprocal. They protect a system from the outside world and protect the outside world from any unintentional signal that a device might radiate.
All of these devices can aid the ECG’s protection circuitry. As this is becoming a complex system, it is wise to simulate it. Free and low-cost calculators5 and simulators6 are available for this task.
The Ultimate Goal Is Patient Protection
There have been many studies concerning the safe current levels impressed across the heart. The standards for medical equipment have bounced around, and today safe levels are less than 4 to 10 µA. This makes the design of medical equipment very demanding with extremely tight margins. Remember too that it is not uncommon to have several pieces of equipment attached to the patient at the same time. The total leakage current, then, must remain below the threshold that can harm the patient’s heart.
With lives in the balance, a designer of defibrillators must understand the entire gamut of possible input protection methods and then choose the best defense at a reasonable cost. Patients must always be protected, which will include proper inspection and calibration of the equipment during the equipment’s lifetime in the medical environment.
References
1. “CPR & Sudden Cardiac Arrest (SCA), Fact Sheet,” American Heart Association, May 8, 2014, http://www.heart.org/HEARTORG/CPRAndECC/WhatisCPR/CPRFactsandStats/CPR-Statistics_UCM_307542_Article.jsp.
2. In medical terms, electrical shocks are usually divided into two categories. Macroshock refers to larger currents (typically more than 10 mA) flowing through a person. These shocks can cause harm or death. Microshock refers to very small currents (as little as 10 to 50 μA) and applies only to the electrically susceptible patient, such as an individual who has an internal conduit that is in direct contact with the heart. This conduit can be a pacing wire or a saline-filled central venous or pulmonary artery catheter. In the electrically susceptible patient, even minute amounts of current (10 μA) can cause ventricular fibrillation. See Barker, Steven J, PhD, MD*; Doyle, D. John, MD, PhD, FRCPC†, “Electrical Safety in the Operating Room: Dry versus Wet,” International Anesthesia Research Society, June 2010, http://journals.lww.com/anesthesia-analgesia/Fulltext/2010/06000/Electrical_Safety_in_the_Operating_Room__Dry.1.aspx. *From the Department of Anesthesiology, University of Arizona College of Medicine, Tucson, Arizona; and †Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland, Ohio.
3. Maxim Integrated application note 639, “Maxim Leads the Way in ESD Protection,” Figures 2 and 3, http://www.maximintegrated.com/app-notes/index.mvp/id/639.
4. Maxim Integrated tutorial 4645, “A Power Engineer: the Super Hero in a Design?” Figure 2, http://www.maximintegrated.com/app-notes/index.mvp/id/4645.
5. At www.maximintegrated.com/cal, see links to Maxim tools and calculators about halfway down the page. The links are to analog design calculators for HP50g with a free PC emulator and a link to an online design and simulator for programmable filters.
6. At www.maximintegrated.com/cal also see links to: Micro-Cap 10 circuit simulator from Spectrum Software (free evaluation version); Solve Elec is a simple circuit simulator (donation software); FilterFree is a filter design program for filters up to three poles (freeware); Kemet Spice Software (freeware); Johanson Technology, JTIsoft (freeware) comprises two advanced design simulation software packages, MLCsoft and MLIsoft, and provides complete S-parameter and SPICE modeling data on Johanson’s line of RF multilayer ceramic capacitors and inductors over the frequency range of 1 MHz to 20 GHz; AADE Filter Design and Analysis (freeware).
Bill Laumeister is an engineer in strategic applications with the Mass Market Solutions Group at Maxim Integrated. He has more than 30 years of experience designing products, helping customers and holds several patents.
About the Author
Bill Laumeister
Bill Laumeister is an engineer in strategic applications at Maxim Integrated Products. He works with customers who use Maxim’s analog and digital integrated circuits. He has more than 30 years of experience and holds several patents.
Voice Your Opinion!
To join the conversation, and become an exclusive member of Electronic Design, create an account today!

Leaders relevant to this article: